|
A Split-Second That Saved My Life
Late one night, halfway from Price to Green River on Highway 6, I was blinded by the unusually bright high beams of an oncoming vehicle. I flashed my lights to signal the driver.
To my shock, the vehicle immediately swerved into my lane.
At a combined speed of over 130 mph, I had no time to think. I instinctively veered onto the shoulder. The truck followed—right into my path again. Moments later, I was completely off the highway, still at full speed.
Then, just as suddenly, it was over. The truck passed. I returned to the road, heart pounding, but unharmed.
What saved me that night is the same system that may now be preventing you from getting better.
Your Body’s Built-In Survival System
In moments of danger, your body activates its fight-or-flight response—part of your autonomic nervous system (ANS), which controls functions you don’t consciously think about.
When this system turns on:
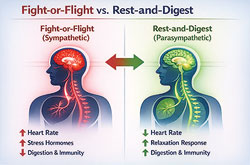 • Your “thinking brain” goes quiet
• Your “thinking brain” goes quiet
• Your reflexes take over
• Blood flow shifts away from digestion, repair,
and immune function
• Every resource is redirected toward survival
It’s fast, automatic, and lifesaving.
Once the danger passes, your system is supposed to shift back into balance—allowing your body to rest, digest, repair, and heal.
When the System Doesn’t Turn Off
But what if it doesn’t?
What if your nervous system gets stuck—partially or fully—in fight-or-flight?
Instead of a temporary survival response, it becomes your baseline.
This is known as sympathetic dominance.
And it’s far more common than most people realize.
In fact, in our clinic, the majority of patients we test show signs of this—even those who say they feel “calm.”
What Stuck in “Fight-or-Flight” Actually Feels Like
If this sounds familiar, you’re not alone:
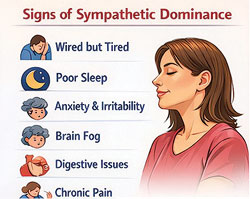 • Feeling “wired but tired” • Feeling “wired but tired”
• Difficulty relaxing or slowing down
• Poor or unrefreshing sleep
• Brain fog or memory issues
• Chronic pain (neck, back, jaw)
• Digestive problems (bloating, reflux, constipation, diarrhea)
• Frequent illness or slow recovery
• Anxiety, overwhelm, or burnout
Some people have no obvious symptoms at all—just high blood pressure or a persistently elevated heart rate.
If you’ve been doing everything “right” and still aren’t getting better, the issue may not be a lack of treatment—it may be a nervous system that isn’t allowing healing to occur.
The Inflammation Connection Most People Miss
The autonomic nervous system doesn’t just control stress—it also plays a major role in regulating inflammation.
The vagus nerve, a key part of the “rest-and-repair” system, helps keep inflammation in check.
When its activity is suppressed—as it often is in sympathetic dominance—inflammation can rise unchecked.
This has been associated with increased risk of conditions such as:
• Heart disease
• Diabetes
• Autoimmune disorders
• Digestive disorders
• Cognitive decline
In other words, a dysregulated nervous system doesn’t just make you feel bad—it can affect nearly every system in your body.
Why Your Autonomic Nervous System Gets Stuck
Sympathetic dominance can be triggered by many things, including:
• Past trauma (physical or emotional)
• Chronic stress
• Hidden infections (gut, mouth, sinuses, etc.)
• Chronic pain
• Major life events (loss, illness, pregnancy)
Sometimes the trigger is obvious. Often, it’s not.
But once the system is stuck, it can stay that way—quietly interfering with healing for years.
How to Reset Your Nervous System Naturally
There are simple, powerful ways to support your nervous system:
• Slow, deep diaphragmatic breathing
• Eating slowly and mindfully
• Limiting screen exposure at night
• Cold exposure (showers or plunges)
• Humming, singing, or gargling
• Yoga, Pilates, or stretching
• Meditation and mindfulness
• Social connection and laughter
• Regular physical activity
• Sunlight exposure
These are effective—but they require consistency, time, and a nervous system that’s able to respond.
When You Need Faster Results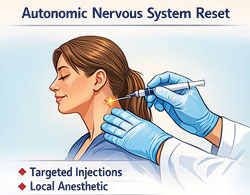
Lifestyle changes are powerful—but they don’t always work quickly, especially if your nervous system is stuck.
In those cases, we offer a procedure called an Autonomic Nervous System Reset.
This involves a series of small, targeted injections just under the skin using a local anesthetic—somewhat similar to acupuncture. The goal is to interrupt abnormal nerve signaling and allow the nervous system to shift back into balance.
In many cases, patients notice changes rapidly—even during the procedure itself. In other cases, they don’t feel different but are finally able to start healing.
If You’re Not Getting Better, This May Be Why
If you’ve been doing everything right—eating well, exercising, taking supplements, trying to manage stress—but still aren’t improving, the issue may not be your effort.
It may be your nervous system.
When your body is no longer stuck in fight-or-flight, healing can finally begin.
If you’d like to learn more about whether you can benefit from a reset, call Prestige Wellness Institute at (435) 259-4466 (Moab) or (435) 210-0184 (Utah County).
|

We often spend our lives taking care of everyone else—kids, partners, and neighbors—but to keep our community strong, we have to prioritize our own well-being, too. From your first check-ups in your 20s to navigating the “change” in your 50s and beyond, your health needs are constantly evolving. Staying on top of regular screenings and simple healthy habits is the best way to prevent chronic conditions and help you feel your best at every stage of life.
Staying on Track: A Guide for Every Age
Maintaining your health is a lifelong journey. Here’s a simple checklist to help you stay on track through the decades:
• Teens and 20s
º Schedule Yearly Check-ups: Establish a relationship with a primary healthcare provider for annual wellness visits.
º Start Cervical Cancer Screenings: Begin regular Pap tests at age 21.
º Prioritize Reproductive Health: Talk openly with your provider about birth control, menstrual health, and STI prevention.
• 30s and 40s
º Stay Consistent: Continue with your yearly physicals and blood pressure checks.
º Begin Mammograms: Start annual breast cancer screenings at age 40 (or earlier if you have a family history).
º Monitor Heart and Bone Health: Pay attention to cholesterol levels and maintain a diet rich in calcium and Vitamin D.
º Track Hormonal Changes: Watch for early signs of perimenopause, such as changes in your sleep, mood, or menstrual cycle.
50s and Beyond
Keep Up with Screenings: Stay current on mammograms and begin colon cancer screenings (typically at age 45 or 50).
Test Bone Density: Ask your provider about a DEXA scan to check for signs of osteoporosis.
Manage Menopause: Talk with your doctor about managing symptoms like hot flashes and maintaining heart health as estrogen levels shift.
Stay Active: Focus on weight-bearing exercises and a healthy diet to support long-term vitality.
Know Your Body, Protect Your Health
Staying healthy isn’t just about “not being sick”—it’s about feeling your best every day. Here are the big areas to keep on your radar:
Heart Health: Heart disease is the leading health concern for women, but the symptoms can be subtle, like extreme fatigue or nausea, rather than just chest pain. Regular checks are your best defense.
Cancer Prevention: Early detection saves lives. Most women should start regular mammograms at age 40 and colon screenings around 45.
Mental Wellness: Women are more likely to experience anxiety or depression, often linked to life transitions or hormonal shifts. Taking care of your mind is just as important as taking care of your heart.
Small Steps, Big Results
You don’t need a total lifestyle overhaul to see a difference. Simply staying active in our beautiful Moab backyard, eating colorful whole foods, and managing stress can go a long way. Most importantly: Don’t skip your annual wellness visit. Think of it as a «tune-up» for your most important vehicle—your body.
Your Partners in Health
Moab Regional Hospital provides primary care and specialty services to support women’s health right here in town. Visiting gynecologist Dr. Kathryn Sarnoski works with our primary care team to offer screenings, reproductive care, and support through all stages of life.
-sharpened.jpg) |
 • Your “thinking brain” goes quiet
• Your “thinking brain” goes quiet