|
|
SCIENCE HAPPENINGS April 2020 |
Coronavirus (COVID-19) Q & A
by Hannah Russell |
I interviewed Katherine Russell, a Registered Nurse that is assisting in preparing a Portland hospital to respond to this pandemic.
Can you give a quick explanation of what Covid19 is?
Coronavirus is a common virus and is the cause of the common cold. “Novel” forms of the virus get introduced into the human population and can cause severe illness. Two novel strains that have been in the news the past decade were MERS and SARS. The name Covid 19 comes from “Coronavirus Disease 2019”. In January 2020 there was an outbreak in Wuhan China where the virus went under-reported and as a result spread rapidly throughout this region in China. The virus can be spread through respiratory droplets when an infected person coughs or sneezes; it also can become aerosolized as a result of different medical procedures. In the community as well as a healthcare setting, droplets can be inhaled into the lungs or absorbed into the tissues of the mouth, nose, or eyes. This strain of Coronavirus is particularly worrisome because of its capacity to cause pneumonia and severe respiratory illness primarily in a select group of the population; this includes immunocompromised individuals and individuals over 60 with other risk factors. It is not quite understood yet why children and healthy adults do not become severely ill when they become infected with this virus. Some individuals show no symptoms and but can still spread the virus.
Will you speak to the life of the virus outside a host?
Public health measures initially centered on identifying sick individuals who had known contact with a sick individual from Wuhan, China. Unfortunately, in February 2020 an individual in California tested positive for Covid 19. This individual did not have a travel history or contact with a known sick individual. This means the virus in now in the community, or “community spread”. Community spread means there is no known source of contact for the disease. When a diseases becomes community spread, it makes public health measures for containment of the disease difficult. The cat is out of the bag, so to speak.
It’s not really known how long the virus lives outside of a host, but best guesses are two to three days. Transmission from a surface to person is possible, you can contaminate your hands by touching a contaminated surface and if the virus reaches your eyes or a mucus membrane. This is the reason why hand washing is such an important preventative measure and you are being told to keep your hands away from your eyes, nose and mouth.
What are best practices for prevention?
Good hand washing, social distancing, keeping hands away from eyes, nose, and mouth, rest, and good nutrition. Stay home if you are sick.

What makes 20 seconds the magic number for washing hands?
Good handwashing involves covering every surface of the hands with soap or hand sanitizer for 20 seconds. This time method and time frame has been shown to substantially decrease the number of germs on the hands. It’s important to clean in between the fingers, the fingertips, palms and the back of the hand. The soap or gel needs contact and time on your skin to kill or reduce the numbers of germs on your hands. Other good tips are to turn on and off the tap with a paper towel, drying your hands thoroughly after washing, and opening the door of public restrooms with a paper towel before throwing it away. Keep work and household surfaces clean.
Does the type of soap matter?
No, there is no difference between the effectiveness of anti-bacterial and regular soap in killing the virus.
What is social distancing? How does it help?
Social distancing is actual space between individuals that reduces the risk of disease transmission. Ideal minimum social distancing between individuals is from three to six feet.
|
 Southeast Utah 500 Women Scientists
Mission and Values: Southeast Utah 500 Women Scientists
Mission and Values:
Our Mission:
• To share the importance of science.
• To support one another as a community of women scientists in Southeast Utah
• To be in service in the name of science to the communities of Southeast Utah.
Our Values
• Being a supportive group for women scientists in Southeast Utah
• Advocate for inclusivity in our group and in science at large
• Increase scientific literacy for locals and tourists
• Mentor and support students of science (especially girls) |
|
$2.5 Million Research Grant Awarded
by Lynnette Harris |
Researchers at Utah State University’s Institute for Antiviral Research in Logan, Utah are at work testing antiviral compounds and licensed drugs for their effectiveness against the novel coronavirus (SARS-CoV-2), the cause of the Covid-19 pandemic. The institute specializes in developing animal models for testing antiviral agents and vaccines and is doing the coronavirus work supported by a $2.5 million research grant from the National Institutes of Health (NIH).
Bart Tarbet, a research associate professor in USU’s Department of Animal, Dairy and Veterinary Sciences (ADVS), is lead investigator on the project, in collaboration with Brett Hurst, ADVS assistant research professor. The scientists will investigate how the virus affects organs and tissues causing disease—a critical step in developing treatments and vaccines—and how the virus responds to various treatments. Institute for Antiviral Research faculty and technicians have been working with the novel coronavirus in test tubes and cell culture plates since late February, and last week finalized the funding for animal model development to investigate possible treatments.
Because of the urgent need to better understand the virus and treat infection, the research team will experiment with different disease models simultaneously, Tarbet said. 
Just as test tubes are not rodents, rodents are not humans, so at each step in the process of gaining approval to treat patients, more compounds are proven ineffective. The researchers recognize there is no perfect model for a disease, but they work to identify the ways in which an infection causes clinical signs in animals that are similar to those in infected humans. That may mean respiratory signs, virus in the blood, or effects on organs that can help identify targets for treatment.
In January, the World Health Organization published a short list of “candidate therapeutic agents” for evaluation against Covid-19 and the USU team has been working with some of those compounds. The NIH added several other potential drugs to the list, including chloroquine and azithromycin that have been mentioned in recent press briefings with the U.S. Coronavirus Task Force. Tarbet pointed out that azithromycin is an antibacterial drug — not an antiviral—suggested to protect against co-infections in patients, but the institute’s previous studies found no benefit from the antibiotic in mice that were infected with influenza virus.
“We also have a database of antiviral compounds from in vitro testing against the 2003 SARS and MERS viruses, so we will be evaluating everything that makes sense to test against this coronavirus,” Tarbet said. “We also work with medicinal chemists from around the world developing potential therapeutic agents. Recently, we have had many research sponsors requesting in vitro testing of new antiviral compounds. We have no shortage of potential drugs to evaluate.”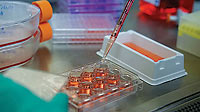
Hurst said, as a virologist, he has been concerned that many social media messages in the early days of Covid-19 tried to minimize its probable impacts with comparisons to rates of illness and death caused by seasonal influenza. Many more people typically get influenza, but the percentage of people who become extremely ill or die is much higher with Covid-19 infections.
He also pointed out that numbers are skewed because people have not been widely tested for the new virus.
“While the number (of deaths) may go down, it is still likely to be higher than influenza and thus it represents a greater threat at this time and something that we definitely need to be vigilant about,” Hurst said.
He added that although scientists and physicians don’t like to speak out about diseases that are not completely understood, he thinks it is important to talk about the dangers of coronavirus and its spread.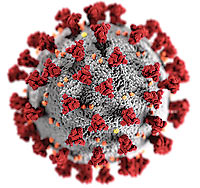
Tarbet, who worked in vaccine development for many years, said in addition to worries about the novel coronavirus, he is concerned about preparations for the 2020 seasonal influenza. Typically this is the time of year, public health leaders and virologists worldwide are making their best predictions for what strain of influenza virus they must prepare to fight the next winter and begin developing and producing sufficient amounts of flu vaccine. This year, they are largely focused on the current crisis.
“What is surprising about this virus is how rapidly it has evolved and spread around the world,” Tarbet said. “I’ve worked with infectious diseases for 25 years, and this is probably the fourth or fifth time that I’ve been involved with an emerging disease, developing vaccines, developing models to test treatments, but none of them have spread this rapidly….It’s almost daily that we’re seeing big changes and almost daily that new discoveries are made, but there are still many things we don’t know the answers to, so we’re working as quickly as we can.” |
|
|
|
|
|
© 2002-2024 Moab Happenings. All rights
reserved.
Reproduction of information contained in this site is
expressly prohibited.
|
|